Abstract
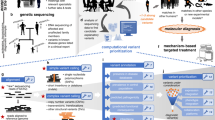
The adaptation of a broad genomic sequencing approach in the clinical setting has been accompanied by considerations regarding the clinical utility, technical performance, and diagnostic yield compared to targeted genetic approaches. We have developed MedExome, an integrated framework for sequencing, variant calling (SNVs, Indels, and CNVs), and clinical assessment of ~4600 medically relevant genes. We compared the technical performance of MedExome with the whole-exome and targeted gene-panel sequencing, assessed the reasons for discordance, and evaluated the added clinical yield of MedExome in a cohort of unresolved subjects suspected of genetic disease. Our analysis showed that despite a higher average read depth in panels (3058 vs. 855), MedExome yielded full coverage of the enriched regions (>20X) and 99% variant concordance rate with panels. The discordance rate was associated with low-complexity regions, high-GC content, and low allele fractions, observed in both platforms. MedExome yielded full sensitivity in detecting clinically actionable variants, and the assessment of 138 patients with suspected genetic conditions resulted in 76 clinical reports (31 full [22.1%], 3 partial, and 42 uncertain/possible molecular diagnoses). MedExome sequencing has comparable performance in variant detection to gene panels. Added diagnostic yield justifies expanded implementation of broad genomic approaches in unresolved patients; however, cost-benefit and health systems impact warrants assessment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Rehm HL. Disease-targeted sequencing: a cornerstone in the clinic. Nat Rev Genet. 2013;14:295.
Shashi V, McConkie-Rosell A, Rosell B, Schoch K, Vellore K, McDonald M, et al. The utility of the traditional medical genetics diagnostic evaluation in the context of next-generation sequencing for undiagnosed genetic disorders. Genet Med. 2014;16:176–82.
Lee H, Deignan JL, Dorrani N, Strom SP, Kantarci S, Quintero-Rivera F, et al. Clinical exome sequencing for genetic identification of rare Mendelian disorders. JAMA. 2014;312:1880–7.
Yavarna T, Al-Dewik N, Al-Mureikhi M, Ali R, Al-Mesaifri F, Mahmoud L, et al. High diagnostic yield of clinical exome sequencing in Middle Eastern patients with Mendelian disorders. Hum Genet. 2015;134:967–80.
Makrythanasis P, Nelis M, Santoni FA, Guipponi M, Vannier A, Béna F, et al. Diagnostic exome sequencing to elucidate the genetic basis of likely recessive disorders in consanguineous families. Hum Mutat. 2014;35:1203–10.
Anagnostopoulou K, Pons R, Dinopoulos A, Vartzelis G, Gika A, Skouteli E, et al. Whole exome sequencing in the diagnosis of neuropaediatric diseases. Eur J Paediatr Neuro. 2017;21:e56.
Stivers T, Timmermans S. The actionability of exome sequencing testing results. Socio Health Illn. 2017;39:1542–56.
Levy MA, Santos S, Kerkhof J, Stuart A, Aref‐Eshghi E, Guo F, et al. Implementation of an NGS‐based sequencing and gene fusion panel for clinical screening of patients with suspected hematologic malignancies. Eur J Hematol. 2019;103:178–89.
Aref-Eshghi E, Kerkhof J, Pedro VP, France GroupeDI, Barat-Houari M, Ruiz-Pallares N, et al. Evaluation of DNA methylation episignatures for diagnosis and phenotype correlations in 42 Mendelian neurodevelopmental disorders. Am J Hum Genet. 2020;106:356–70.
Lanktree MB, Sadikovic B, Waye JS, Levstik A, Lanktree BB, Yudin J, et al. Clinical evaluation of a hemochromatosis next‐generation sequencing gene panel. Eur J Hematol. 2017;98:228–34.
Schenkel LC, Kerkhof J, Stuart A, Reilly J, Eng B, Woodside C, et al. Clinical next-generation sequencing pipeline outperforms a combined approach using sanger sequencing and multiplex ligationdependent probe amplification in targeted gene panel analysis. J Mol Diagn. 2016;18:657–67.
Kerkhof J, Schenkel LC, Reilly J, McRobbie S, Aref-Eshghi E, Stuart A, et al. Clinical validation of copy number variant detection from targeted next-generation sequencing panels. J Mol Diagn. 2017;19:905–20.
Li H. Aligning sequence reads, clone sequences and assembly contigs with BWA-MEM. arXiv. 2013;1303:3997.
Li H, Handsaker B, Wysoker A, Fennell T, Ruan J, Homer N, et al. 1000 Genome Project Data Processing Subgroup. The sequence alignment/map format and SAMtools. Bioinformatics. 2009;25:2078–9.
Lai Z, Markovets A, Ahdesmaki M, Chapman B, Hofmann O, McEwen R, et al. VarDict: a novel and versatile variant caller for nextgeneration sequencing in cancer research. Nucleic Acids Res. 2016;44:e108.
Sandmann S, De Graaf AO, Karimi M, Van Der Reijden BA, Hellström-Lindberg E, Jansen JH, et al. Evaluating variant calling tools for non-matched next-generation sequencing data. Sci Rep. 2017;7:43169.
Mandelker D, Schmidt RJ, Ankala A, Gibson KM, Bowser M, Sharma H, et al. Navigating highly homologous genes in a molecular diagnostic setting: a resource for clinical next-generation sequencing. Genet Med. 2016;18:1282.
Ye K, Schulz MH, Long Q, Apweiler R, Ning Z. Pindel: a pattern growth approach to detect break points of large deletions and medium sized insertions from paired-end short reads. Bioinformatics. 2009;25:2865–71.
Pajusalu S, Pfundt R, Vissers LE, Kwint MP, Reimand T, Õunap K, et al. Identifying long indels in exome sequencing data of patients with intellectual disability. bioRxiv. 2018;244756.
Plagnol V, Curtis J, Epstein M, Mok KY, Stebbings E, Grigoriadou S, et al. A robust model for read count data in exome sequencing experiments and implications for copy number variant calling. Bioinformatics. 2012;28:2747–54.
Ellingford JM, Campbell C, Barton S, Bhaskar S, Gupta S, Taylor RL, et al. Validation of copy number variation analysis for next-generation sequencing diagnostics. Eur J Hum Genet. 2017;25:719–24.
Sund KL, Rehder CW. Detection and reporting of homozygosity associated with consanguinity in the clinical laboratory. Hum Herd. 2014;77:217–24.
Sund KL, Zimmerman SL, Thomas C, Mitchell AL, Prada CE, Grote L, et al. Regions of homozygosity identified by SNP microarray analysis aid in the diagnosis of autosomal recessive disease and incidentally detect parental blood relationships. Genet Med. 2013;15:70.
Morgan M, Pagès H, Obenchain V, Hayden N. Rsamtools: binary alignment (BAM), FASTA, variant call (BCF), and tabix file import. R package version 2.4.0. http://bioconductor.org/packages/Rsamtools. Accessed 19 Sep 2020.
Conrad DF, Pinto D, Redon R, Feuk L, Gokcumen O, Zhang Y, et al. Origins and functional impact of copy number variation in the human genome. Nature. 2010;464:704.
Girdea M, Dumitriu S, Fiume M, Bowdin S, Boycott KM, Chénier S, et al. PhenoTips: patient phenotyping software for clinical and research use. Hum Mutat. 2013;34:1057–65.
Richards S, Aziz N, Bale S, Bick D, Das S, Gastier-Foster J, et al. ACMG Laboratory Quality Assurance Committee. Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet Med. 2015;17:405.
Wright CF, Prigmore E, Rajan D, Handsaker J, McRae J, Kaplanis J, et al. Clinically-relevant postzygotic mosaicism in parents and children with developmental disorders in trio exome sequencing data. Nat Commun. 2019;10:2985.
Yang R, Nelson AC, Henzler C, Thyagarajan B, Silverstein KA. ScanIndel: a hybrid framework for indel detection via gapped alignment, split reads and de novo assembly. Genome Med. 2015;7:127.
Monroe GR, Frederix GW, Savelberg SM, De Vries TI, Duran KJ, Van Der Smagt JJ, et al. Effectiveness of whole-exome sequencing and costs of the traditional diagnostic trajectory in children with intellectual disability. Genet Med. 2016;18:949.
Timmermans S, Tietbohl C, Skaperdas E. Narrating uncertainty: variants of uncertain significance (VUS) in clinical exome sequencing. BioSocieties. 2017;12:439–58.
Cummings BB, Marshall JL, Tukiainen T, Lek M, Donkervoort S, Foley AR, et al. Improving genetic diagnosis in Mendelian disease with transcriptome sequencing. Sci Transl Med. 2017;9:eaal5209.
Aref-Eshghi E, Bend EG, Colaiacovo S, Caudle M, Chakrabarti R, Napier M, et al. Diagnostic utility of genome-wide DNA methylation testing in genetically unsolved individuals with suspected hereditary conditions. Am J Hum Genet. 2019;104:685–700.
Aref‐Eshghi E, Bourque DK, Kerkhof J, Carere DA, Ainsworth P, Sadikovic B, et al. Genome‐wide DNA methylation and RNA analyses enable reclassification of two variants of uncertain significance in a patient with clinical Kabuki syndrome. Hum Mutat. 2019;40:1684–9.
Aref-Eshghi E, Schenkel LC, Lin H, Skinner C, Ainsworth P, Paré G, et al. Clinical validation of a genome-wide DNA methylation assay for molecular diagnosis of imprinting disorders. J Mol Diagn. 2017;19:848–56.
Aref-Eshghi E, Rodenhiser DI, Schenkel LC, Lin H, Skinner C, Ainsworth P, et al. Genomic DNA methylation signatures enable concurrent diagnosis and clinical genetic variant classification in neurodevelopmental syndromes. Am J Hum Genet. 2018;102:156–74.
Aref-Eshghi E, Schenkel LC, Lin H, Skinner C, Ainsworth P, Paré G, et al. The defining DNA methylation signature of Kabuki syndrome enables functional assessment of genetic variants of unknown clinical significance. Epigenetics. 2017;12:923–33.
Bend EG, Aref-Eshghi E, Everman DB, Rogers RC, Cathey SS, Prijoles EJ, et al. Gene domain-specific DNA methylation episignatures highlight distinct molecular entities of ADNP syndrome. Clin Epigenet. 2019;11:64.
Aref-Eshghi E, McGee JD, Pedro VP, Kerkhof J, Stuart A, Ainsworth PJ, et al. Genetic and epigenetic profiling of BRCA1/2 in ovarian tumors reveals additive diagnostic yield and evidence of a genomic BRCA1/2 DNA methylation signature. J Hum Genet. 2020. https://doi.org/10.1038/s10038-020-0780-4.
Schenkel LC, Aref-Eshghi E, Skinner C, Ainsworth P, Lin H, Paré G, et al. Peripheral blood epi-signature of Claes-Jensen syndrome enables sensitive and specific identification of patients and healthy carriers with pathogenic mutations in KDM5C. Clin Epigenet. 2018;10:21.
Krzyzewska IM, Maas SM, Henneman P, vd Lip K, Venema A, Baranano K, et al. A genome-wide DNA methylation signature for SETD1B-related syndrome. Clin Epigenet. 2019;11:156.
Ciolfi A, Aref-Eshghi E, Pizzi S, Pedace L, Miele E, Kerkhof J, et al. Frameshift mutations at the C-terminus of HIST1H1E result in a specific DNA hypomethylation signature. Clin Epigenet. 2020;12:7.
Aref-Eshghi E, Schenkel LC, Ainsworth P, Lin H, Rodenhiser DI, Cutz JC, et al. Genomic DNA methylation-derived algorithm enables accurate detection of malignant prostate tissues. Front Oncol. 2018;8:100.
Aref-Eshghi E, Bend EG, Hood RL, Schenkel LC, Carere DA, Chakrabarti R, et al. BAFopathies’ DNA methylation epi-signatures demonstrate diagnostic utility and functional continuum of Coffin– Siris and Nicolaides–Baraitser syndromes. Nat Commun. 2018;9:4885.
Acknowledgements
The authors would like to thank the staff and physicians at the medical genetics clinic at London Health Science Centre, ON, Canada for recruiting the patients into the study, as well as the patients and their families for their support.
Funding
This study was supported by the London Health Sciences Centre Pathology and Laboratory Medicine Research and Innovation Fund.
Author information
Authors and Affiliations
Contributions
EA-E: bioinformatics, variant assessment, and manuscript writing; JK: Sample processing and sequencing; DAC, MV, HL, and TB: variant assessment; PB: manuscript writing; SC, MS, MC, NK, CP, TB, CC, and VMS: patient recruitment and clinical assessment; BS: principal investigator and supervision of the research team.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
The study protocol has been approved by the Western University Research Ethics Board (REB 108261).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Aref-Eshghi, E., Kerkhof, J., Carere, D.A. et al. Clinical and technical assessment of MedExome vs. NGS panels in patients with suspected genetic disorders in Southwestern Ontario. J Hum Genet 66, 451–464 (2021). https://doi.org/10.1038/s10038-020-00860-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s10038-020-00860-3
This article is cited by
-
Clinical pharmacogenetic analysis in 5,001 individuals with diagnostic Exome Sequencing data
npj Genomic Medicine (2022)