Abstract
Objective
To characterize the rate of monitoring alarms by alarm priority, signal type, and developmental age in a Level-IIIB Neonatal Intensive Care Unit (NICU) population.
Study design
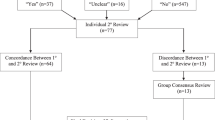
Retrospective analysis of 2,294,687 alarm messages from Philips monitors in a convenience sample of 917 NICU patients, covering 12,001 patient-days. We stratified alarm rates by alarm priority, signal type, postmenstrual age (PMA) and birth weight (BW), and reviewed and adjudicated over 21,000 critical alarms.
Results
Of all alarms, 3.6% were critical alarms, 55.0% were advisory alarms, and 41.4% were device alerts. Over 60% of alarms related to oxygenation monitoring. The average alarm rate (±SEM) was 177.1 ± 4.9 [median: 135.9; IQR: 89.2–213.3] alarms/patient-day; the medians varied significantly with PMA and BW (p < 0.001) in U-shaped patterns, with higher rates at lower and higher PMA and BW. Based on waveform reviews, over 99% of critical arrhythmia alarms were deemed technically false.
Conclusions
The alarm burden in this NICU population is very significant; the average alarm rate significantly underrepresents alarm rates at low and high PMA and BW. Virtually all critical arrhythmia alarms were artifactual.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Change history
25 July 2018
The previously published version of this Article contained an error in Fig. 1 where the “HR low” and “HR high” labels were swapped.
Furthermore, in Table 1 of this Article, the fifth row in the centre column contained a typographical error where the study population birth weight incorrectly read “2050 (1 450–2 650)”, rather than “2050 (1450–2650)”.
These errors have now been corrected in both the PDF and HTML versions of the Article.
References
Tsien CL, Fackler JC. Poor prognosis for existing monitors in the intensive care unit. Crit Care Med. 1997;25(4):614–9.
Johnson KR, Hagadorn JI, Sink DW. Alarm safety and alarm fatigue. Clin Perinatol. 2017;44(3):713–28.
Paine CW, Goel VV, Ely E, Stave CD, Stemler S, Zander M, et al. Systematic review of physiologic monitor alarm characteristics and pragmatic interventions to reduce alarm frequency. J Hosp Med. 2016;11(2):136–44.
Association for the Advancement of Medical Instrumentation. Clinical Alarms—2011 summit. Arlington, VA: Association for the Advancement of Medical Instrumentation; 2011.
Cvach M. Monitor alarm fatigue: an integrative review. Biomed Instrum Technol. 2012;46(4):268–77.
Vergales BD, Paget-Brown AO, Lee H, Guin LE, Smoot TJ, Rusin CG, et al. Accurate automated apnea analysis in preterm infants. Am J Perinatol. 2014;31(2):157–62.
Joshi R, van Pul C, Atallah L, Feijs L, Van Huffel S, Andriessen P. Pattern discovery in critical alarms originating from neonates under intensive care. Physiol Meas. 2016;37(4):564–79.
van Pul C, VDM HP, VDB JJ, Mohns, Andriessen T, Safe P. Patient monitoring is challenging, but still feasible in a neonatal intensive care unit with single family rooms. Acta Paediatr. 2015;104(6):e247–54.
Ketko AK, Martin CM, Nemshak MA, Niedner M, Vartanian RJ. Balancing the tension between hyperoxia prevention and alarm fatigue in the NICU. Pediatrics. 2015;136(2):e496–504.
McClure C, Jang SY, Fairchild K. Alarms, oxygen saturations, and SpO2 averaging time in the NICU. J Neonatal Perinat Med. 2016;9(4):357–62.
Saeed M, Villarroel M, Reisner AT, Clifford G, Lehman LW, Moody G, et al. Multiparameter intelligent monitoring in intensive care II: a public-access intensive care unit database. Crit Care Med. 2011;39(5):952–60.
The WFDB Software Package. Software for viewing, analyzing, and creating recordings of physiologic signals. http://physionet.org/physiotools/wfdb.shtml (2015) Accessed 4 January 2015.
IntelliVue patient monitor MP 20/30, MP 40/50, MP 60/70/90 – instructions for use. Philips Healthcare, Germany; 2005.
The Joint Commmission. 2017 National Patient Safety Goals. https://www.jointcommission.org/hap_2017_npsgs/ Accessed 2017 May 25
Schondelmeyer AC, Bonafide CP, Goel VV, Blake N, Cvach M, Sucharew H, et al. The frequency of physiologic monitor alarms in a children’s hospital. J Hosp Med. 2016;11(11):796–8.
Ahlborn V, Bohnhorst B, Peter CS, Poets CF. False alarms in very low birthweight infants: comparison between three intensive care monitoring systems. Acta Paediatr. 2000;89(5):571–6.
Sahni R, Gupta A, Ohira-Kist K, Rosen TS. Motion resistant pulse oximetry in neonates. Arch Dis Child Fetal Neonatal Ed. 2003;88(6):F505–508.
Stefanescu BM, O’Shea TM, Haury F, Carlo WA, Slaughter JC. Improved filtering of pulse oximeter monitoring alarms in the neonatal ICU: bedside significance. Respir Care. 2016;61(1):85–89.
Cvach MM, Biggs M, Rothwell KJ, Charles-Hudson C. Daily electrode change and effect on cardiac monitor alarms: an evidence-based practice approach. J Nurs Care Qual. 2013;28(3):265–71.
Sendelbach S, Wahl S, Anthony A, Shotts P. Stop the noise: a quality improvement project to decrease electrocardiographic nuisance alarms. Crit Care Nurse. 2015;35(4):15–22.
Rheineck-Leyssius AT, Kalkman CJ. Influence of pulse oximeter settings on the frequency of alarms and detection of hypoxemia: Theoretical effects of artifact rejection, alarm delay, averaging, median filtering or a lower setting of the alarm limit. J Clin Monit Comput. 1998;14(3):151–6.
Gorges M, Markewitz BA, Westenskow DR. Improving alarm performance in the medical intensive care unit using delays and clinical context. Anesth Analg. 2009;108(5):1546–52.
Vagedes J, Poets CF, Dietz K. Averaging time, desaturation level, duration and extent. Arch Dis Child Fetal Neonatal Ed. 2013;98(3):F265–66.
Zong W, Moody GB, Mark RG. Reduction of false arterial blood pressure alarms using signal quality assessment and relationships between the electrocardiogram and arterial blood pressure. Med Biol Eng Comput. 2004;42(5):698–706.
Aboukhalil A, Nielsen L, Saeed M, Mark RG, Clifford GD. Reducing false alarm rates for critical arrhythmias using the arterial blood pressure waveform. J Biomed Inform. 2008;41(3):442–51.
Acknowledgements
The authors wish to thank Mr. Jeffrey Smith, Clinical Engineering, BIDMC, for his help and support over the course of this study. Additionally, the authors thank Mr. Nirmal Balachundhar, Mr. Rémi Dekimpe, Ms. Tiffany Ho, and Ms. Nalini Singh for their help with the adjudication of bedside monitoring alarms. The data collection and archiving was supported in part through grants R01 EB001659 and R01 GM104987 from the National Institute of Biomedical Imaging and Bioengineering and National Institute of General Medical Sciences, respectively, of the United States National Institutes of Health. The data analysis was supported in part by Nihon Kohden Corporation and Nihon Kohden Innovation Center, and in part by a Massachusetts Institute of Technology (MIT) Peter J. Eloranta Summer Undergraduate Research Fellowship and the MIT-Wertheimer Undergraduate Research and Innovation Scholar Fund. Preliminary analyses of this work were presented as a poster at the 2016 Pediatric Academic Societies Annual Meeting in Baltimore, MD.
Author contributions
TL led the data analysis, interpreted the results, helped draft the initial manuscript, critically reviewed and revised the manuscript, and approved the final manuscript as submitted. MM contributed to the data analysis, interpreted the results, helped draft and critically review and revise the initial manuscript, and approved the final manuscript as submitted. WT and SY provided clinical perspective on the study, interpreted the results, critically reviewed and revised the initial manuscript, and approved the final manuscript as submitted. DM supported the clinical data extraction and data collection, critically reviewed the initial manuscript, and approved the final manuscript as submitted. MG contributed to and supported the data collection, provided clinical perspective on the study, interpreted the results, critically reviewed and revised the initial manuscript, and approved the final manuscript as submitted. TH conceptualized, designed, and supervised all aspects of the study, including data collection, data analysis, overall study progress, and drafting and revising of the manuscript. He critically reviewed the manuscript and approved the final manuscript as submitted.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
TH has received research funding from the National Institutes of Health, Nihon Kohden Corporation, Maxim Integrated, and Philips Healthcare. MM remained a salaried employee of Nihon Kohden Corporation while contributing to this study as a Visiting Scientist at MIT’s Institute for Medical Engineering & Science. TL received partial internship support from Nihon Kohden Innovation Center. SY, DM, WT, and MG declare no potential conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Li, T., Matsushima, M., Timpson, W. et al. Epidemiology of patient monitoring alarms in the neonatal intensive care unit. J Perinatol 38, 1030–1038 (2018). https://doi.org/10.1038/s41372-018-0095-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-018-0095-x
This article is cited by
-
Clinical feasibility of an advanced neonatal epidermal multiparameter continuous monitoring technology in a large public maternity hospital in Nairobi, Kenya
Scientific Reports (2022)
-
Management of oxygen saturation monitoring in preterm newborns in the NICU: the Italian picture
Italian Journal of Pediatrics (2021)