Abstract
Objective
To examine the association between haemoglobin (Hb) concentrations in mothers before and during pregnancy and those in children at 3–5 years of age.
Methods
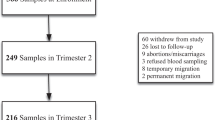
The study included 78,923 women who conceived during 1993–1996 and delivered a singleton live infant. Maternal Hb concentrations were measured at pre-pregnancy health check-up and first prenatal visit, and during the second and third trimester. Hb concentrations of children born to these women were measured at 3–5 years of age. Associations between Hb levels in mothers and children were examined. Unconditional logistic regression was used to explore the association between maternal Hb levels and risk for anaemia in children.
Results
Maternal Hb levels before and during pregnancy were positively associated with children’s Hb levels. Using maternal Hb ≥ 130 g/L as the referent, the risk for anaemia in children at 3–5 years of age was higher when maternal second trimester Hb concentrations were 70–99 g/L (odds ratio [OR] = 1.76, 95% confidence interval [CI] = 1.56–1.99), 100–109 g/L (OR = 1.45, 95% CI = 1.29–1.64), and 110–119 g/L (OR = 1.18, 95% CI = 1.04–1.33). Children were 1.52 and 1.23-times more likely to suffer from anaemia when maternal third trimester Hb concentrations were 70–99 and 100–109 g/L, respectively. A pre-pregnancy Hb concentration of 80–109 g/L and first prenatal visit Hb concentrations of 80–109 and 100–119 g/L were also associated with increased risks for childhood anaemia.
Conclusion
Low maternal Hb concentrations before or during pregnancy increase the risk for anaemia in children at 3–5 years of age.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Balarajan Y, Ramakrishnan U, Ozaltin E, Shankar AH, Subramanian SV. Anaemia in low-income and middle-income countries. Lancet. 2011;378:2123–35. https://doi.org/10.1016/s0140-6736(10)62304-5.
Hipgrave DB, Fu X, Zhou H, Jin Y, Wang X, Chang S, et al. Poor complementary feeding practices and high anaemia prevalence among infants and young children in rural central and western China. Eur J Clin Nutr. 2014;68:916–24. https://doi.org/10.1038/ejcn.2014.98.
Gao W, Yan H, Wang D, Dang S, Pei L. Severity of anemia among children under 36 months old in rural western China. PLoS ONE. 2013;8:e62883 https://doi.org/10.1371/journal.pone.0062883.
Eneroth H, Persson LA, El Arifeen S, Ekstrom EC. Infant anaemia is associated with infection, low birthweight and iron deficiency in rural Bangladesh. Acta Paediatr. 2011;100:220–5. https://doi.org/10.1111/j.1651-2227.2010.02011.x.
Koura GK, Ouedraogo S, Le Port A, Watier L, Cottrell G, Guerra J, et al. Anaemia during pregnancy: impact on birth outcome and infant haemoglobin level during the first 18 months of life. Trop Med Int Health. 2012;17:283–91. https://doi.org/10.1111/j.1365-3156.2011.02932.x.
Kilbride J, Baker TG, Parapia LA, Khoury SA, Shuqaidef SW, Jerwood D. Anaemia during pregnancy as a risk factor for iron-deficiency anaemia in infancy: a case-control study in Jordan. Int J Epidemiol. 1999;28:461–8.
Zhang Y, Jin L, Liu JM, Ye R, Ren A. Maternal hemoglobin concentration during gestation and risk of anemia in infancy: secondary analysis of a randomized controlled trial. J Pediatr. 2016;175:106. https://doi.org/10.1016/j.jpeds.2016.05.011.
Berry RJ, Li Z, Erickson JD, Li S, Moore CA, Wang H, et al. Prevention of neural-tube defects with folic acid in China. China–U.S. collaborative project for neural tube defect prevention. N Engl J Med. 1999;341:1485–90. https://doi.org/10.1056/nejm199911113412001.
Li H, Ye R, Pei L, Ren A, Zheng X, Liu J. Caesarean delivery, caesarean delivery on maternal request and childhood overweight: a Chinese birth cohort study of 181 380 children. Pediatr Obes. 2014;9:10–16. https://doi.org/10.1111/j.2047-6310.2013.00151.x.
World Health Organisation. Haemoglobin concentrations for the diagnosis of anaemia and assessment of severity. Geneva: Vitamin and mineral nutrition information system (VMNIS); 2011. http://www.who.int/vmnis/indicators/haemoglobin.pdf. Accessed 4 Feb. 2018.
De Pee S, Bloem MW, Sari M, Kiess L, Yip R, Kosen S. The high prevalence of low hemoglobin concentration among Indonesian infants aged 3-5 months is related to maternal anemia. J Nutr. 2002;132:2215–21.
Blouin B, Penny ME, Maheu-Giroux M, Casapia M, Aguilar E, Silva H, et al. Timing of umbilical cord-clamping and infant anaemia: the role of maternal anaemia. Paediatr Int Child Health. 2013;33:79–85. https://doi.org/10.1179/2046905512y.0000000036.
Maketa V, Mavoko HM, da Luz RI, Zanga J, Lubiba J, Kalonji A, et al. The relationship between Plasmodium infection, anaemia and nutritional status in asymptomatic children aged under five years living in stable transmission zones in Kinshasa, Democratic Republic of Congo. Malar J. 2015;14:83 https://doi.org/10.1186/s12936-015-0595-5.
Rawat R, Saha KK, Kennedy A, Rohner F, Ruel M, Menon P. Anaemia in infancy in rural Bangladesh: contribution of iron deficiency, infections and poor feeding practices. Br J Nutr. 2014;111:172–81. https://doi.org/10.1017/s0007114513001852.
Gonzales GF. Hemoglobin and testosterone: importance on high altitude acclimatization and adaptation. Rev Peru De Med Exp y Salud Publica. 2011;28:92–100.
Tran TD, Fisher J, Hanieh S, Tran T, Simpson JA, Tran H, et al. Antenatal iron supplementation regimens for pregnant women in rural Vietnam and subsequent haemoglobin concentration and anaemia among their infants. PLoS ONE. 2015;10:e0125740 https://doi.org/10.1371/journal.pone.0125740.
Viteri FE. Iron endowment at birth: maternal iron status and other influences. Nutr Rev. 2011;69(Suppl 1):S3–16. https://doi.org/10.1111/j.1753-4887.2011.00449.x.
Braithwaite VS, Prentice A, Darboe MK, Prentice AM, Moore SE. The effects of maternal iron deficiency on infant fibroblast growth factor-23 and mineral metabolism. Bone. 2016;83:1–8. https://doi.org/10.1016/j.bone.2015.10.003.
Dai AI, Demiryurek S, Aksoy SN, Perk P, Saygili O, Gungor K. Maternal iron deficiency anemia as a risk factor for the development of retinopathy of prematurity. Pediatr Neurol. 2015;53:146–50. https://doi.org/10.1016/j.pediatrneurol.2015.04.002.
Barker DJ, Gluckman PD, Godfrey KM, Harding JE, Owens JA, Robinson JS. Fetal nutrition and cardiovascular disease in adult life. Lancet. 1993;341:938–41.
Harvey NC, Poole JR, Javaid MK, Dennison EM, Robinson S, Inskip HM, et al. Parental determinants of neonatal body composition. J Clin Endocrinol Metab. 2007;92:523–6. https://doi.org/10.1210/jc.2006-0456.
Entringer S, Kumsta R, Nelson EL, Hellhammer DH, Wadhwa PD, Wust S. Influence of prenatal psychosocial stress on cytokine production in adult women. Dev Psychobiol. 2008;50:579–87. https://doi.org/10.1002/dev.20316.
Entringer S, Wust S, Kumsta R, Layes IM, Nelson EL, Hellhammer DH, et al. Prenatal psychosocial stress exposure is associated with insulin resistance in young adults. Am J Obstet Gynecol. 2008;199:498.e491–497. https://doi.org/10.1016/j.ajog.2008.03.006.
Zerfu TA, Umeta M, Baye K. Dietary diversity during pregnancy is associated with reduced risk of maternal anemia, preterm delivery, and low birth weight in a prospective cohort study in rural Ethiopia. Am J Clin Nutr. 2016;103:1482–8. https://doi.org/10.3945/ajcn.115.116798.
Backstrand JR, Allen LH, Black AK, de Mata M, Pelto GH. Diet and iron status of nonpregnant women in rural Central Mexico. Am J Clin Nutr. 2002;76:156–64.
Zimmermann MB, Chaouki N, Hurrell RF. Iron deficiency due to consumption of a habitual diet low in bioavailable iron: a longitudinal cohort study in Moroccan children. Am J Clin Nutr. 2005;81:115–21.
Horton S. The economics of food fortification. J Nutr. 2006;136:1068–71.
Wilunda C, Tanaka S, Esamai F, Kawakami K. Prenatal anemia control and anemia in children aged 6–23 months in sub-Saharan Africa. Matern Child Nutr. 2016. https://doi.org/10.1111/mcn.12375
Martorell R, Ascencio M, Tacsan L, Alfaro T, Young MF, Addo OY, et al. Effectiveness evaluation of the food fortification program of Costa Rica: impact on anemia prevalence and hemoglobin concentrations in women and children. Am J Clin Nutr. 2015;101:210–7. https://doi.org/10.3945/ajcn.114.097709.
Zhang CM, Zhao WY, Gao AX, Su TT, Wang YK, Zhang YQ, et al. How could agronomic biofortification of rice be an alternative strategy with higher cost-effectiveness for human iron and zinc deficiency in China? Food Nutr Bull. 2017. doi:https://doi.org/10.1177/0379572117745661.
Acknowledgements
All authors read and approved the final manuscript. The original project was supported by a cooperative agreement between the US Centers for Disease Control and Prevention and Peking University (grant No. U01 DD000293).
Author contributions
AR conceived the study and revised the manuscript; YZ analysed the data and wrote the first draft; LJ provided critical comments on the first draft; JL and RY supervised the follow-up study. No honorarium, grant, or other form of payment was given to anyone to produce the manuscript. AR takes primary responsibility for the final content.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Zhang, Y., Jin, L., Liu, Jm. et al. Maternal haemoglobin concentrations before and during pregnancy as determinants of the concentrations of children at 3–5 years of age: A large follow-up study. Eur J Clin Nutr 73, 1102–1109 (2019). https://doi.org/10.1038/s41430-018-0284-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-018-0284-x