Abstract
Purpose
To evaluate the efficacy of infliximab (IFX, 5–10 mg/kg) (Group 1) and tocilizumab (TCZ, 4–8 mg/kg) (Group 2) infusions in non-infectious retinal vasculitis (RV) using Angiographic Scoring for the Uveitis Working Group fluorescein angiography (FA) scoring system.
Methods
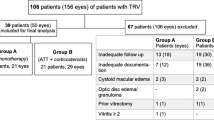
Records of 14 patients (24 eyes) in Group 1 and 8 patients (11 eyes) in Group 2 were retrospectively evaluated to assess visual acuity (VA), anterior chamber cell and flare, vitreous haze, central subfield thickness (CST), and FA scoring at baseline and 6 months of follow-up. The measurements were employed to grade in each group.
Results
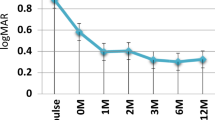
In Group 1 and 2, respectively, there was no underlying disease in 9 (60%) and 3 (42.9%) patients. Three (42.9%) patients in Group 2 had juvenile idiopathic arthritis (JIA) as the most common identified cause. Mean improvement in VA (log MAR) and CST were 0.04 ± 0.14 and 40.3 ± 78.5 µm in Group 1; 0.04 ± 0.09 and 47.3 ± 82.3 µm in Group 2, respectively. Mean FA scores were significantly reduced from 12.4 ± 5.2 and 11.6 ± 4.4 at baseline to 6.4 ± 5.0 and 5.8 ± 3.9 at 6-month in Group 1 and 2, respectively. In Group 2, 9 eyes of 6 patients (75%) had the history of IFX use prior to TCZ initiation. There was no significant safety concern requiring treatment discontinuation during the follow-up in either group.
Conclusion
IFX and TCZ infusions showed statistically significant improvement of non-infectious RV as shown by ASUWOG FA Scoring System. TCZ, as well as IFX, appeared to be effective treatment options for non-infectious RV.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are only available from the corresponding author on reasonable request.
References
Jabs DA, Nussenblatt RB, Rosenbaum JT. Standardization of Uveitis Nomenclature Working G. Standardization of uveitis nomenclature for reporting clinical data. Results of the First International Workshop. Am J Ophthalmol. 2005;140:509–16. https://doi.org/10.1016/j.ajo.2005.03.057.
Abu El-Asrar AM, Herbort CP, Tabbara KF. Retinal vasculitis. Ocul Immunol Inflamm. 2005;13:415–33. https://doi.org/10.1080/09273940591003828.
El-Asrar AM, Herbort CP, Tabbara KF. A clinical approach to the diagnosis of retinal vasculitis. Int Ophthalmol. 2010;30:149–73. https://doi.org/10.1007/s10792-009-9301-3.
Ciardella AP, Prall FR, Borodoker N, Cunningham ET Jr. Imaging techniques for posterior uveitis. Curr Opin Ophthalmol. 2004;15:519–30. https://doi.org/10.1097/01.icu.0000144386.05116.c5.
Tugal-Tutkun I, Herbort CP, Khairallah M, Angiography Scoring for Uveitis Working G. Scoring of dual fluorescein and ICG inflammatory angiographic signs for the grading of posterior segment inflammation (dual fluorescein and ICG angiographic scoring system for uveitis). Int Ophthalmol. 2010;30:539–52. https://doi.org/10.1007/s10792-008-9263-x.
Suhler EB. A prospective trial of infliximab therapy for refractory uveitis: preliminary safety and efficacy outcomes. Arch Ophthalmol. 2005;123:903–12. https://doi.org/10.1001/archopht.123.7.903.
Kang HM, Lee SC. Long-term progression of retinal vasculitis in Behcet patients using a fluorescein angiography scoring system. Graefes Arch Clin Exp Ophthalmol. 2014;252:1001–8. https://doi.org/10.1007/s00417-014-2637-z.
Balci O, Jeannin B, Herbort CP Jr. Contribution of dual fluorescein and indocyanine green angiography to the appraisal of posterior involvement in birdshot retinochoroiditis and Vogt-Koyanagi-Harada disease. Int Ophthalmol. 2018;38:527–39. https://doi.org/10.1007/s10792-017-0487-5.
Sadiq MA, Hassan M, Afridi R, Halim MS, Do DV, Sepah YJ, et al. Posterior segment inflammatory outcomes assessed using fluorescein angiography in the STOP-UVEITIS study. Int J Retin Vitreous. 2020;6:47. https://doi.org/10.1186/s40942-020-00245-w
Hatemi G, Silman A, Bang D, Bodaghi B, Chamberlain AM, Gul A, et al. EULAR recommendations for the management of Behcet disease. Ann Rheum Dis. 2008;67:1656–62. https://doi.org/10.1136/ard.2007.080432.
Rosenbaum JT, Sibley CH, Lin P. Retinal vasculitis. Curr Opin Rheumatol. 2016;28:228–35. https://doi.org/10.1097/BOR.0000000000000271.
Calvo-Río V, Blanco R, Beltrán E, Sánchez-Bursón J, Mesquida M, Adán A, et al. Anti-TNF-alpha therapy in patients with refractory uveitis due to Behcet’s disease: a 1-year follow-up study of 124 patients. Rheumatol (Oxf). 2014;53:2223–31. https://doi.org/10.1093/rheumatology/keu266.
Sharma PK, Markov GT, Bajwa A, Foster CS. Long-Term Efficacy of Systemic Infliximab in Recalcitrant Retinal Vasculitis. Retina. 2015;35:2641–6. https://doi.org/10.1097/IAE.0000000000000624.
Eser Ozturk H, Oray M, Tugal-Tutkun I. Tocilizumab for the Treatment of Behcet Uveitis that Failed Interferon Alpha and Anti-Tumor Necrosis Factor-Alpha Therapy. Ocul Immunol Inflamm. 2018;26:1005–14. https://doi.org/10.1080/09273948.2017.1355471
Atienza-Mateo B, Calvo-Rio V, Beltran E, Martinez-Costa L, Valls-Pascual E, Hernandez-Garfella M, et al. Anti-interleukin 6 receptor tocilizumab in refractory uveitis associated with Behcet’s disease: multicentre retrospective study. Rheumatol (Oxf). 2018;57:856–64. https://doi.org/10.1093/rheumatology/kex480.
Fabiani C, Sota J, Rigante D, Vitale A, Emmi G, Lopalco G, et al. Efficacy of adalimumab and infliximab in recalcitrant retinal vasculitis inadequately responsive to other immunomodulatory therapies. Clin Rheumatol. 2018;37:2805–9. https://doi.org/10.1007/s10067-018-4133-z.
Calvo-Río V, Santos-Gómez M, Calvo I, González-Fernández MI, López-Montesinos B, Mesquida M, et al. Anti-Interleukin-6 Receptor Tocilizumab for Severe Juvenile Idiopathic Arthritis-Associated Uveitis Refractory to Anti-Tumor Necrosis Factor Therapy: A Multicenter Study of Twenty-Five Patients. Arthritis Rheumatol. 2017;69:668–75. https://doi.org/10.1002/art.39940.
Muselier A, Bielefeld P, Bidot S, Vinit J, Besancenot JF, Bron A. Efficacy of tocilizumab in two patients with anti-TNF-alpha refractory uveitis. Ocul Immunol Inflamm. 2011;19:382–3. https://doi.org/10.3109/09273948.2011.606593.
Wennink RAW, Ayuso VK, de Vries LA, Vastert SJ, de Boer JH. Tocilizumab as an Effective Treatment Option in Children with Refractory Intermediate and Panuveitis. Ocul Immunol Inflamm. 2021;29:21–25. https://doi.org/10.1080/09273948.2020.1712431.
Ucan Gunduz G, Yalcinbayir O, Cekic S, Yildiz M, Kilic SS. Anti-Tumor Necrosis Factor Treatment in the Management of Pediatric Noninfectious Uveitis: Infliximab Versus Adalimumab. J Ocul Pharm Ther. 2021;37:236–40. https://doi.org/10.1089/jop.2020.0081.
Santos-Gómez M, Calvo-Río V, Blanco R, Beltrán E, Mesquida M, Adán A, et al. The effect of biologic therapy different from infliximab or adalimumab in patients with refractory uveitis due to Behcet’s disease: results of a multicentre open-label study. Clin Exp Rheumatol 2016;34:S34–S40.
Ashkenazy N, Saboo US, Abraham A, Ronconi C, Cao JH. Successful treatment with infliximab after adalimumab failure in pediatric noninfectious uveitis. J AAPOS. 2019;23:151 e1–151 e5. https://doi.org/10.1016/j.jaapos.2019.02.006.
Maleki A, Garcia CM, Asgari S, Manhapra A, Foster CS Response to the Second TNF-alpha Inhibitor (Adalimumab or Infliximab) after Failing the First One in Refractory Idiopathic Inflammatory Retinal Vascular Leakage. Ocul Immunol Inflamm. 2021:1-10. https://doi.org/10.1080/09273948.2020.1869787.
Sepah YJ, Sadiq MA, Chu DS, Dacey M, Gallemore R, Dayani P, et al. Primary (Month-6) Outcomes of the STOP-Uveitis Study: Evaluating the Safety, Tolerability, and Efficacy of Tocilizumab in Patients With Noninfectious Uveitis. Am J Ophthalmol. 2017;183:71–80. https://doi.org/10.1016/j.ajo.2017.08.019.
Maleki A, Manhapra A, Asgari S, Chang PY, Foster CS, Anesi SD. Tocilizumab Employment in the Treatment of Resistant Juvenile Idiopathic Arthritis Associated Uveitis. Ocul Immunol Inflamm. 2021;29:14–20. https://doi.org/10.1080/09273948.2020.1817501.
Farhat R, Clavel G, Villeneuve D, Abdelmassih Y, Sahyoun M, Gabison E, et al. Sustained Remission with Tocilizumab in Refractory Relapsing Polychondritis with Ocular Involvement: A Case Series. Ocul Immunol Inflamm. 2021;29:9–13. https://doi.org/10.1080/09273948.2020.1763405.
Adán A, Mesquida M, Llorenç V, Espinosa G, Molins B, Hernández MV, et al. Tocilizumab treatment for refractory uveitis-related cystoid macular edema. Graefes Arch Clin Exp Ophthalmol. 2013;251:2627–32. https://doi.org/10.1007/s00417-013-2436-y.
Vegas-Revenga N, Calvo-Rio V, Mesquida M, Adan A, Hernandez MV, Beltran E, et al. Anti-IL6-Receptor Tocilizumab in Refractory and Noninfectious Uveitic Cystoid Macular Edema: Multicenter Study of 25 Patients. Am J Ophthalmol. 2019;200:85–94. https://doi.org/10.1016/j.ajo.2018.12.019.
Paul S, Zhang X. Small sample GEE estimation of regression parameters for longitudinal data. Stat Med. 2014;33:3869–81. https://doi.org/10.1002/sim.6198.
Mesquida M, Molins B, Llorenc V, Sainz de la Maza M, Adan A. Long-term effects of tocilizumab therapy for refractory uveitis-related macular edema. Ophthalmology. 2014;121:2380–6. https://doi.org/10.1016/j.ophtha.2014.06.050.
Haraoui B, Cameron L, Ouellet M, White B. Anti-infliximab antibodies in patients with rheumatoid arthritis who require higher doses of infliximab to achieve or maintain a clinical response. J Rheumatol. 2006;33:31–6.
Acknowledgements
IK was supported by a grant from the International Council of Ophthalmology (ICO) Retina Research Foundation (RRF) Helmerich Fellowship Program, as the recipient of 2020 ICO-RRF Helmerich One-Year Fellowship Award. WM was supported by a grant from the Japan Eye Bank Association Oversea Research Program and Kobe University Long Term Oversea Visit Program for Young Researchers.
Funding
Research to Prevent Blindness Department Challenge Award and National Eye Institute of the National Institutes of Health P30 Award (EY026877) have been awarded to the Byers Eye Institute at Stanford University.
Author information
Authors and Affiliations
Contributions
IK was responsible for conducting the research, designing the study, extracting and analyzing the data, interpreting the results, writing and revising the manuscript; GU contributed in extracting the data, editing and critical revision of the manuscript; WM was responsible for analyzing the data, interpreting the results, critical revision of the manuscript; JR was responsible for editing and revision of the manuscript; CO contributed in interpreting the data and critical revision of the manuscript; AM contributed in interpreting the data; MSH contributed to design of the study and data interpretation; MZ contributed in analyzing and interpreting the data; SL was responsible for extracting the data; AD was responsible for extracting the data; HG contributed in analyzing and interpreting the data, editing and critical revision of the manuscript; QDN was responsible for critical revision of the manuscript.
Corresponding author
Ethics declarations
Competing interests
QDN serves on the Scientific Advisory Board for Affibody, Acelyrin, and Regeneron. The remaining authors declare that there are no conflicts of interest related to this manuscript.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Karaca, I., Uludag, G., Matsumiya, W. et al. Six-month outcomes of infliximab and tocilizumab therapy in non-infectious retinal vasculitis. Eye 37, 2197–2203 (2023). https://doi.org/10.1038/s41433-022-02315-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-022-02315-9
This article is cited by
-
Human retinal endothelial cells express functional interleukin-6 receptor
Journal of Ophthalmic Inflammation and Infection (2023)