Abstract
Critical limb ischemia (CLI) has a poor prognosis and adversely affects patients’ quality of life (QOL). Therapeutic angiogenesis may improve mobility, mortality and QOL in CLI patients. However, the effectiveness of gene therapy on such patients’ QOL is unknown. DVC1-0101, a non-transmissible recombinant Sendai virus vector expressing human fibroblast growth factor-2 gene, demonstrated safety and efficacy in a phase I/II study of CLI patients. We investigated the effects of DVC1-0101 on QOL in this cohort. QOL was assessed using the Short Form-36 health survey version 2 (SF-36) in 12 patients at pre-administration, 28 days and 3, 6 and 12 months post-treatment. We examined differences between pre and post-administration QOL scores and correlations between QOL scores and vascular parameters. Patients demonstrated low baselines scores on every SF-36 dimension. Post-treatment scores showed significant improvements in physical functioning at 3 and 6 months (P < 0.05), role-physical at 3, 6 and 12 months (P < 0.05), bodily pain at 1, 3, 6 and 12 months (P < 0.05), vitality at 1, 6 and 12 months (P < 0.05) and physical component summary at 6 and 12 months (P < 0.05). DVC1-0101-based gene therapy may improve QOL in CLI patients over a 6-month period.
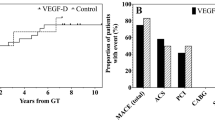
Similar content being viewed by others
Introduction
Peripheral arterial disease (PAD) affects the arteries in the limbs and comprises a range of conditions caused by stenosis or occlusive atherosclerosis in the vascular bed1. PAD affects around 12% of the adult population and thus represents an important public health issue2. PAD progression is associated with reduced quality of life (QOL) due to limited mobility because of pain in the lower legs during walking (intermittent claudication). Intermittent claudication progresses to critical limb ischemia (CLI) in approximately one in four patients within 5 years3. CLI induces pain at rest and ischemic leg ulcers/gangrene, with substantial deterioration in QOL. Mortality is as high as 20% and major amputation is required within 1 year in 40% of patients with CLI4. Although advanced surgical and endovascular techniques exist, many patients are ineligible5 and there is currently no effective pharmacologic therapy for CLI, resulting in the need for amputation in many patients.
The poor prognosis and increasing morbidity and mortality of CLI indicate the need for new therapies, including gene therapy, aimed at inducing angiogenesis6. The use of gene therapy to induce angiogenesis was initially proposed in the late 1990 s and has since become a potentially attractive clinical option for the treatment of PAD7,8. Fibroblast growth factor-2 (FGF-2) is one of the most promising angiogenic growth factors. It was recognized as an angiogenic factor based on its induction of endothelial cell proliferation, migration and morphogenesis, extracellular matrix degradation and vessel maturation9. Furthermore, recombinant Sendai virus has been identified as an efficient gene carrier for FGF-2, allowing pronounced angiogenesis10,11,12. Unlike other gene-transfer virus vectors, Sendai virus is a cytoplasmic, negative-stranded RNA virus that replicates entirely in the cytoplasm of cells, with no DNA intermediate. DVC1-0101 is a new RNA gene drug based on a non-transmissible recombinant Sendai virus carrying the FGF-2 gene, which was investigated in a first-in-man gene therapy clinical trial in CLI patients who were ineligible for standard vascular interventions (‘no-option’ CLI) completed in March 201113.
CLI patients experience significant limitations in terms of their physical functioning and functional status, thus, improving their QOL, as well as their clinical status, has become a vital treatment goal in these patients14. However, innovative gene therapy is still in the early clinical trial phase and QOL data are therefore lacking. The current study investigated the effects of gene therapy using DVC1-0101 on QOL measures in 12 patients with CLI, initially treated in the above study13.
Results
Patient characteristics
A total of 12 patients were enrolled with a mean age of 65.0 ± 11.38 years (range 48–82 years), as described previously13. The majority of patients were male (83%) and 75% had a history of smoking. Ten patients were diagnosed with arteriosclerosis obliterans and two with thromboangiitis obliterans. Three patients had ulcers on their ankles and/or toes at enrolment. According to Fontaine grade, 75% were grade III and the rest were grade IV. SF-36 data were available for all 12 participants.
Baseline SF-36 data for all the participants are summarized in Supplementary Table S1. The mean (±standard deviation) pain level was 2.67 (±0.89) according to the 5-point Likert scale. The mean ankle–brachial index (ABI) was 0.49 (±0.31) mmHg and the mean absolute claudication distance (ACD) based on the eight patients eligible for the treadmill test was 126.13 (±93.88) m. Of the 12 participants, nine had a medical history of re-vascularization, five had a history and/or comorbid myocardial infarction or angina and six had a medical history of stroke.
Norm-based QOL scores
All the patients demonstrated low scores in every dimension of SF-36 at baseline (Fig. 1). Mean norm-based scoring (NBS) scores were below those of the general population in all dimensions. The poorest scores obtained were in the physical health domain, including physical functioning and role-physical. The low physical component summary and role/social component summary scores reflected the patients’ overall poor physical health.
Differences in Short Form-36 health survey scores in 12 patients with critical limb ischemia compared with Japanese national standards.
The Short Form-36 health survey includes eight domains: physical functioning (PF); role-physical (RP); bodily pain (BP); general health (GH); vitality (VT); social functioning (SF); role-emotional (RE); and mental health (MH). Abbreviation: SD, standard deviation.
SF-36 NBS physical functioning and role/social component summary scores were significantly higher in TAO patients compared with ASO patients (P = 0.0302 and P = 0.0317, respectively). SF-36 NBS scores were also significantly lower in Fontaine grade III compared with grade IV in terms of vitality (P = 0.0122), role-emotional (P = 0.0295), mental health (P = 0.0441) and mental component summary (P = 0.0335) (Table 1).
Effect of gene therapy on QOL score
Amputation strongly affects patient QOL and the two patients who underwent amputation after administration of DVC1-0101 were therefore excluded from the analysis of treatment effectiveness (Table 2). There were significant improvements in physical functioning at 3 months (P = 0.0098) and 6 months (P = 0.042), in role-physical at 3 months (P = 0.0078), 6 months (P = 0.002) and 12 months (P = 0.0195), in bodily pain at 1 month (P = 0.0469), 3 months (P = 0.0039), 6 months (P = 0.0078) and 12 months (P = 0.0391), in vitality at 1 month (P = 0.0273), 6 months (P = 0.043) and 12 months (P = 0.0313) and in physical component summary at 6 months (P = 0.0322) and 12 months (P = 0.0068).
Overall summary measures for all 12 participants revealed significant improvements in physical component summary at 6 months (P = 0.032) and 12 months (P = 0.0105) after administration of DVC1-0101 (Fig. 2). There was no dose-related effect of DVC1-0101 on QOL, except in terms of physical functioning and mental health, which both improved more in the low-dose (5 × 107 and 2 × 108 cell infections units/60 kg body weight) compared with the high-dose (1 × 109 and 5 × 109 cell infectious units/60 kg body weight) groups (Table 3).
Overall summary measures of the Short Form-36 health survey for all 12 patients with critical limb ischemia.
The eight domains of the Short Form-36 health survey can be aggregated into three summary measures: physical component summary (PCS); mental component summary (MCS); and role/social component summary (RCS).
Correlations between QOL score and vascular parameters
We analysed the correlations between baseline factors and improvements in SF-36 measures after administration of gene therapy by paired t-tests. Age over 65 years was significantly associated with improvements in mental component summary (Supplementary Table S2). There were no differences in summary scores in relation to diagnosis, sex, Fontaine grade, medical history of myocardial infarction, or dose. There were no positive correlations between improvements in changes of SF-36 summary scores and changes of ACD, ABI and pain scales after DVC1-0101 administration. There were, however, positive correlations between physical component summary and toe–brachial index (TBI) and thermography (r = 0.88 and r = 0.86, respectively; P = 0.001) (Supplementary Table S3).
Discussion
Therapeutic angiogenesis for PAD using proteins, cells with angiogenic properties and angiogenic genes, has been examined extensively over the past two decades. However, no modality has shown definitive clinical benefit, including in terms of QOL. DVC1-0101 is a recombinant Sendai virus-based RNA gene drug that provides a novel gene-delivery system for strong expression of the native FGF-2 gene. Preclinical studies of DVC1-0101 have demonstrated local peak FGF-2 protein concentrations in muscles of >10-fold control levels11,12. FGF-2 was the first angiogenic factor shown to improve walking performance in PAD patients15 and Sendai virus-expressed FGF-2 demonstrated excellent limb-salvaging effects compared with other factors and vectors11,12. We therefore conducted a first-in-man phase I/IIa study to evaluate the safety and efficacy of DVC1-010113. The current study assessed SF-36-based QOL in these patients and found that post-treatment QOL scores for physical functioning, role-physical, bodily pain, vitality and physical component summary were significantly improved after administration of DVC1-0101. It must be noted that these results are extracted from a phase I/IIa, single-arm study, with no randomization and no-placebo control. Thus, the findings are preliminary and must be interpreted with caution; however, the results are suggestive of DVC1-0101 possibly showing some effectiveness at improving QOL in patients with no-option CLI.
PAD is associated with reduced walking ability, reduced physical and mental functional statuses and QOL compared with patients without PAD16. Ischemic leg pain limits activities and thus tends to isolate patients from social connections, with consequent stagnating effects on emotional and mental health. Baseline reference QOL data for patients with no-option CLI using SF-36 NBS reported low scores in every dimension14. Similarly, patients in the current study with no-option CLI demonstrated scores well below the mean for the general population in all dimensions. These low QOL scores suggest that patients with CLI need help to improve or preserve their QOL.
The severity of PAD has previously been reported to have a significant impact on QOL17. QOL is often indicated by walking performance in patients with intermittent claudication. A phase II, randomized, double-blind, placebo-controlled RAVE study concluded that there was no significant improvement in QOL in patients with predominantly unilateral intermittent claudication who underwent adenoviral vascular endothelial growth factor gene transfer compared with placebo, according to the walking impairment questionnaire and SF-3618. The phase II TRAFFIC study demonstrated that the primary outcome of change in peak walking time significantly increased in patients treated with single-dose compared with placebo, though improved walking ability did not affect QOL15. However, angiogenesis gene therapy is still in an experimental stage and results are based on early-phase clinical trials; further late-phase trials are therefore needed to examine the effects of angiogenesis on QOL in relation to walking function in patients with intermittent claudication.
Improving QOL for patients with CLI may be more challenging. QOL assessment using SF-36 in patients with CLI who underwent revascularization, major amputation, or conservative treatment failed to show any significant improvement19. Furthermore, although angioplasty significantly increased QOL scores in patients with intermittent claudication, no such improvement was seen in patients with CLI20. In contrast, Shigematsu et al.21 reported significant improvements in SF-36 measures, especially in terms of body pain and mental health dimensions, in CLI patients treated with hepatocyte growth factor plasmid compared with placebo in a phase III trial, with primary endpoints of rest pain and reduction of ulcer size21. The significant reductions in rest pain and ulcer size in this study suggest that QOL in terms of body pain and mental health dimensions increased.
Physical functioning scores improved significantly in the current study at 3 and 6 months after DVC1-0101 administration and the physical component summary score improved significantly at 12 months. These findings suggest that it is possible that DVC1-0101 may effectively preserve or improve long-term QOL in patients with CLI. The factors associated with treatment-related improvements in QOL remain unclear. DVC1-0101 was shown to be safe, well-tolerated and to improve walking function significantly13; however, the current study found no significant correlation between QOL and change in ACD. Furthermore, although an association between disease-related pain and QOL has been reported20, no such relationship was identified in the current study. Similarly, there was no dose-related effect of DVC1-0101 on QOL, suggesting that even low-dose DVC1-0101 may effectively improve or preserve long-term QOL in patients with CLI. The significant improvements observed in QOL at certain time points after administration of DVC1-0101 indicate its future potential for improving QOL in patients with CLI.
The strength of this study was its experimental design and its role as the first clinical study of the effects of gene therapy with DVC1-0101 on QOL in patients with CLI. However, the small sample size, single-arm and dose-escalation study design limits the ability to generalize from the results and further randomized, late-phase trials are needed to confirm the value of these preliminary results. Data concerning the effects of angiogenesis on QOL are currently limited and the implications of the current study are ambivalent with regard to the roles of angiogenesis and angioplasty in relation to different staging classifications of PAD.
In conclusion, this study suggests the ability of gene therapy using DVC1-0101 to preserve or improve long-term QOL in patients with CLI. The increasing availability of gene therapy thus holds great promise for the future treatment of CLI.
Methods
Patients and study design
QOL data for CLI patients who were enrolled in a single-centre, phase I/IIa, open-label, four-dose-escalating trial of DVC1-0101 were used in this study13. The study was conducted in Japan from 2006 to 2010 and all the participants originated from the same geographic area. Twelve CLI patients were divided into four dose cohorts (n = 3 each) who received 5 × 107, 2 × 108, 1 × 109 and 5 × 109 cell infectious units/60 kg body weight, respectively, in a dose-escalating manner. They were observed for 6 months and followed-up for up to 12 months. DVC1-0101 was administered at 30 sites with varying ischemic conditions in one limb per patient. The Japanese Guidelines for Clinical Trials of Gene Therapy issued by the Ministry of Health, Labour and Welfare require that only ‘no-option’ patients may be enrolled in first-in-man gene therapy studies and only CLI patients in whom standard vascular interventions were contraindicated were therefore eligible to participate. Other inclusion criteria were a diagnosis of arteriosclerosis obliterans or thromboangiitis obliterans, with no evidence of malignancies, unstable cardiovascular disease, immunodeficiencies, or haemodialysis. Nine patients had a history of smoking, but enrolment required them to stop smoking at least 1 month before screening13.
Short Form-36 health survey and NBS
The Short Form-36 version 2 (SF-36) health survey was used to evaluate QOL, including measures of health improvement, treatment effectiveness and comparisons of disease burden across populations22,23,24. SF-36 includes eight domains: physical functioning, role-physical, bodily pain, general health, vitality, social functioning, role-emotional and mental health. These eight domains can be aggregated into three summary measures: physical component summary, mental component summary and role/social component summary. The QOL scores were evaluated using a NBS method that delivered standardized scores such that the mean general population scores were set at 50 for every dimension. The NBS score was calculated using the 2007 Japanese population norms as representative. SF-36 has been shown to be reliable and has been validated worldwide and its Japanese version has also been validated22,23,24. SF-36 was performed pre-administration and at 28 days and 3, 6 and 12 months after gene administration.
Physiological parameters
ABI and TBI are indicators of the haemodynamics in the lower legs and toes. These indexes are calculated as the ratio between the highest blood pressure in the right or left brachial artery and the highest blood pressure in the posterior tibial or dorsalis pedis and toes25. An ABI <0.9 mmHg indicates leg ischemia. ABI and TBI were measured as a potential correlational variable using an automatic oscillometric system (VS-1500A; Fukuoka Denshi, Tokyo, Japan). Pulse-volume recording was measured using the same oscillometric system and rated using a 3-point grading scale: − = flat, + = slight pulsation and ++ = normal pulsation. ACD and change in ACD as measures of walking function were assessed using a treadmill test. Eight patients were eligible for the flat-slope test at 2.4 km/h, which was terminated at 300 m to avoid the risk of cardiovascular complications. ABI and ACD were measured pre-administration as baseline and every month up to 12 months after gene therapy administration. Pain was rated using a 5-point Likert scale to measure the level of pain in the ischemic legs at rest: 1 = no pain, 2 = pain sometimes, 3 = occasionally need pain medication, 4 = always need pain medication and 5 = cannot sleep at night even with pain medication. The laser Doppler perfusion index was measured using a laser Doppler perfusion index analyser (Moor Instruments, Denver, UK) and data only from the treated leg were used in the current study. Blinded dermatologists used thermography to measure the temperature of the skin of the feet, controlling for constant room temperature and allowing an interval after the removal of the patients’ socks and shoes. Differences in foot pad temperatures were calculated in degrees Celsius by subtracting the temperature of the untreated limb from the temperature of the treated limb.
Ethics
Ethical approval for this clinical trial was granted by the Kyushu University Institutional Review Board for Clinical Trials, the Health Sciences Council of the Japan Ministry of Health, Labour and Welfare and Biosafety Committees, according to national regulations and approved guidelines. Written informed consent was obtained from all subjects before data collection. This trial was registered with University Hospital Medical Information Network Center (Tokyo, Japan), UMIN-ID C000000404.
Data analysis
SF-36 QOL scores were calculated using the Japanese SF-36 scoring program (v.3; QualityMetric Inc., Lincoln, RI, USA). Differences in baseline QOL scores in relation to characteristic variables were analysed by one-way analysis of variance (ANOVA). Differences between QOL scores before and after administration of DVC1-0101 and dose-related effects on QOL were analysed by Wilcoxon’s signed-rank tests. The influences of characteristic variables on the effects of DVC1-0101 on QOL were investigated by one-way ANOVA. Pearson’s correlation coefficient was used to examine the correlations between increases in QOL and ACD, ABI and pain scale pre- and post-administration. Values of P < 0.05 were considered significant. All analyses were carried out using the Statistical Package for JMP software (v.11; SAS Institute Inc., Cary, NC, USA).
Additional Information
How to cite this article: Matsumoto, T. et al. Improved quality of life in patients with no-option critical limb ischemia undergoing gene therapy with DVC1-0101. Sci. Rep. 6, 30035; doi: 10.1038/srep30035 (2016).
References
Mughal, N. A., Russell, D. A., Ponnambalam, S. & Homer-Vanniasinkam, S. Gene therapy in the treatment of peripheral arterial disease. Br J Surg 99, 6–15 (2012).
Madonna, R. & Rokosh, G. Insights into gene therapy for critical limb ischemia: the devil is in the details. Vascul Pharmacol 57, 10–14 (2012).
Tiong, A. & Freedman, S. B. Gene therapy for cardiovascular disease: the potential of VEGF. Curr Opin Mol Ther 6, 151–159 (2004).
Takeshita, S. et al. Therapeutic angiogenesis: a single intraarterial bolus of vascular endothelial growth factor augments revascularization in a rabbit ischemic hind limb model. J Clin Invest 93, 662–670 (1994).
Sedighiani, F. & Nikol, S. Gene therapy in vascular disease. Surgeon 9, 326–335 (2011).
Davies, M. G. Critical limb ischemia: cell and molecular therapies for limb salvage. Methodist Debakey Cardiovasc J 8, 20–27 (2012).
Germani, A., Di Campli, C., Pompilio, G., Biglioli, P. & Capogrossi, M. C. Regenerative therapy in peripheral artery disease. Cardiovasc Ther 27, 289–304 (2009).
Baumgartner, I. et al. Constitutive expression of phVEGF165 after intramuscular gene transfer promotes collateral vessel development in patients with critical limb ischemia. Circulation 97, 1114–1123 (1998).
Presta, M. et al. Fibroblast growth factor/fibroblast growth factor receptor system in angiogenesis. Cytokine Growth Factor Rev 16, 159–178 (2005).
Yonemitsu, Y. et al. Efficient gene transfer to airway epithelium using recombinant Sendai virus. Nat Biotechnol 18, 970–973 (2000).
Masaki, I. et al. Angiogenic gene therapy for experimental critical limb ischemia: acceleration of limb loss by overexpression of VEGF165 but not of FGF-2. Circ Res 90, 966–973 (2002).
Onimaru, M. et al. Fibroblast growth factor-2 gene transfer can stimulate hepatocyte growth factor expression irrespective of hypoxia-mediated downregulation in ischemic limbs. Circ Res 91, 923–930 (2002).
Yonemitsu, Y. et al. DVC1-0101 to treat peripheral arterial disease: a phase I/IIa open-label dose-escalation clinical trial. Mol Ther 21, 707–714 (2013).
Sprengers, R. W. et al. Quality of life in patients with no-option critical limb ischemia underlines the need for new effective treatment. J Vasc Surg 52, 843–849 (2010).
Lederman, R. J. et al. Therapeutic angiogenesis with recombinant fibroblast growth factor-2 for intermittent claudication (the TRAFFIC study): a randomized trial. Lancet 359, 2053–2058 (2002).
Killewich, L. A. Improving functional status and quality of life in elderly patients with peripheral arterial disease. J Am Coll Surg 202, 345–355 (2006).
Amer, M. S., Alsadany, M. A., Tolba, M. F. & Omer, O. H. Quality of life in elderly diabetic patients with peripheral arterial disease. Geriatr Gerontol Int 13, 443–450 (2013).
Rajagopalan, S. et al. Regional angiogenesis with vascular endothelial growth factor in peripheral arterial disease: a phase II randomized, double-blind, controlled study of adenoviral delivery of vascular endothelial growth factor 121 in patients with disabling intermittent claudication. Circulation 108, 1933–1938 (2003).
Hernandez-Osma, E., Cairols, M. A., Marti, X., Barjau, E. & Riera, S. Impact of treatment on the quality of life in patients with critical limb ischaemia. Eur J Vasc Endovasc Surg 23, 491–494 (2002).
Culverwell, A. D., Tapping, C. R., Ettles, D. F. & Kessel, D. Patient experience, pain and quality of life after lower limb angioplasty: a multisite prospective cohort study. Cardiovasc Intervent Radiol 35, 788–794 (2012).
Shigematsu, H. et al. Randomized, double-blind, placebo-controlled clinical trial of hepatocyte growth factor plasmid for critical limb ischemia. Gene Ther 17, 1152–1161 (2010).
Fukuhara, S., Bito, S., Green, J., Hisako, A. & Kurokawa, K. Translation, adaptation and validation of the SF-36 Health Survey for use in Japan. J Clin Epidemiol 51, 1037–1044 (1998).
Fukuhara, S., Ware, J. E., Kosinski, M., Wada, S. & Gandek, B. Psychometric and clinical tests of validity of the Japanese SF-36 Health Survey. J Clin Epidemiol 51, 1045–1053 (1998).
Suzukamo, Y. et al. Validation testing of a three-component model of Short Form-36 scores. J Clin Epidemiol 64, 3 (2011).
Aboyans, V. et al. Measurement and interpretation of the ankle-brachial index: a scientific statement from the American Heart Association. Circulation 126, 2890–2909 (2012).
Acknowledgements
This study was supported in part by a Health Labour Sciences Research Grant and by the Japan Agency for Medical Research and Development.
Author information
Authors and Affiliations
Contributions
Y.Y. conceived and designed the experiments; T.M., K.Y., R.Y. and Y.M. performed the experiments and prepared tables and figures; K.H.-Y. collected the sample data; M.T. contributed to the writing of the manuscript; Y.M. and Y.Y. reviewed the manuscript; all authors contributed to the writing of the manuscript and discussed the manuscript at various stages.
Ethics declarations
Competing interests
Dr. Yonemitsu was a previous member of the scientific advisory board of DNAVEC Corporation, which has developed DVC1-0101. The other authors declare that they have no conflicts of interest.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Matsumoto, T., Tanaka, M., Yoshiya, K. et al. Improved quality of life in patients with no-option critical limb ischemia undergoing gene therapy with DVC1-0101. Sci Rep 6, 30035 (2016). https://doi.org/10.1038/srep30035
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep30035
This article is cited by
-
Gene therapy research in Asia
Gene Therapy (2017)
-
ETV-2 activated proliferation of endothelial cells and attenuated acute hindlimb ischemia in mice
In Vitro Cellular & Developmental Biology - Animal (2017)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.