Abstract
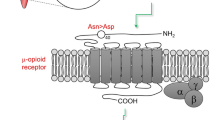
The μ1 opioid receptor (OPRM1) genetic variant A118G results in decreased μ-receptor binding potential in the brain and increases morphine requirement. We hypothesized that OPRM1 A118G polymorphism will affect morphine-induced respiratory depression (MIRD) risk in children receiving morphine. A prospective genotype-blinded study was conducted in 88 healthy adolescents (11–18 years; 67% female, 85% Caucasian) who underwent spine fusion for scoliosis. They were followed for 48 h postoperatively for MIRD, pain scores, morphine consumption and use of analgesic adjuvants. Patients were genotyped for OPRM1 A118G variant—76% were wild type (AA) and 24% heterozygous/homozygous for variant (AG/GG). Multivariable logistic regression showed that the risk of MIRD in patients with AA genotype was significantly higher (odds ratio 5.6, 95% CI: 1.4–37.2, P=0.030). Presence of G allele was associated with higher pain scores (effect size 0.73, P=0.045). This novel association is an important step toward predicting MIRD susceptibility and personalizing morphine use.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Overdyk FJ, Carter R, Maddox RR, Callura J, Herrin AE, Henriquez C . Continuous oximetry/capnometry monitoring reveals frequent desaturation and bradypnea during patient-controlled analgesia. Anesth Analg 2007; 105: 412–418.
Voepel-Lewis T, Marinkovic A, Kostrzewa A, Tait AR, Malviya S . The prevalence of and risk factors for adverse events in children receiving patient-controlled analgesia by proxy or patient-controlled analgesia after surgery. Anesth Analg 2008; 107: 70–75.
Sadhasivam S, Boat A, Mahmoud M . Comparison of patient-controlled analgesia with and without dexmedetomidine following spine surgery in children. J Clin Anesth 2009; 21: 493–501.
Fecho K, Jackson F, Smith F, Overdyk FJ . In-hospital resuscitation: opioids and other factors influencing survival. Therapeut Clin Risk Manag 2009; 5: 961–968.
Overdyk FJ . Postoperative opioids remain a serious patient safety threat. Anesthesiology 2010; 113: 259–260.
Lotsch J, Dudziak R, Freynhagen R, Marschner J, Geisslinger G . Fatal respiratory depression after multiple intravenous morphine injections. Clin Pharmacokinet 2006; 45: 1051–1060.
Brennan F, Carr DB, Cousins M . Pain management: a fundamental human right. Anesth Analg 2007; 105: 205–221.
Liu SS, Wu CL . Effect of postoperative analgesia on major postoperative complications: a systematic update of the evidence. Anesth Analg 2007; 104: 689–702.
Duarte LT, Fernandes Mdo C, Costa VV, Saraiva RA . The incidence of postoperative respiratory depression in patients undergoing intravenous or epidural analgesia with opioids. Br J Anestesiol 2009; 59: 409–420.
Bouwmeester NJ, Anderson BJ, Tibboel D, Holford NH . Developmental pharmacokinetics of morphine and its metabolites in neonates, infants and young children. Br J Anaesth 2004; 92: 208–217.
Sadhasivam S, Chidambaran V, Ngamprasertwong P, Esslinger HR, Prows C, Zhang X et al. Race and unequal burden of perioperative pain and opioid related adverse effects in children. Pediatrics 2012; 129: 832–838.
Angst MS, Lazzeroni LC, Phillips NG, Drover DR, Tingle M, Ray A et al. Aversive and reinforcing opioid effects: a pharmacogenomic twin study. Anesthesiology 2012; 117: 22–37.
Angst MS, Phillips NG, Drover DR, Tingle M, Ray A, Swan GE et al. Pain sensitivity and opioid analgesia: a pharmacogenomic twin study. Pain 2012; 153: 1397–1409.
Dahan A, Aarts L, Smith TW . Incidence, reversal, and prevention of opioid-induced respiratory depression. Anesthesiology 2010; 112: 226–238.
Dahan A, Sarton E, Teppema L, Olievier C, Nieuwenhuijs D, Matthes HW et al. Anesthetic potency and influence of morphine and sevoflurane on respiration in mu-opioid receptor knockout mice. Anesthesiology 2001; 94: 824–832.
Huang P, Chen C, Mague SD, Blendy JA, Liu-Chen LY . A common single nucleotide polymorphism A118G of the mu opioid receptor alters its N-glycosylation and protein stability. Biochem J 2012; 441: 379–386.
Chou WY, Wang CH, Liu PH, Liu CC, Tseng CC, Jawan B . Human opioid receptor A118G polymorphism affects intravenous patient-controlled analgesia morphine consumption after total abdominal hysterectomy. Anesthesiology 2006; 105: 334–337.
Chou WY, Yang LC, Lu HF, Ko JY, Wang CH, Lin SH et al. Association of mu-opioid receptor gene polymorphism (A118G) with variations in morphine consumption for analgesia after total knee arthroplasty. Acta Anaesthesiol Scand 2006; 50: 787–792.
Sia AT, Lim Y, Lim EC, Goh RW, Law HY, Landau R et al. A118G single nucleotide polymorphism of human mu-opioid receptor gene influences pain perception and patient-controlled intravenous morphine consumption after intrathecal morphine for postcesarean analgesia. Anesthesiology 2008; 109: 520–526.
Tan EC, Lim EC, Teo YY, Lim Y, Law HY, Sia AT . Ethnicity and OPRM variant independently predict pain perception and patient-controlled analgesia usage for post-operative pain. Mol Pain 2009; 5: 32.
Walter C, Lotsch J . Meta-analysis of the relevance of the OPRM1 118A>G genetic variant for pain treatment. Pain 2009; 146: 270–275.
Sadhasivam S, Ganesh A, Robison A, Kaye R, Watcha MF . Validation of the bispectral index monitor for measuring the depth of sedation in children. Anesth Analg 2006; 102: 383–388.
Voepel-Lewis T, Burke CN, Jeffreys N, Malviya S, Tait AR . Do 0-10 numeric rating scores translate into clinically meaningful pain measures for children? Anesth Analg 2011; 112: 415–421.
Gauderman W, Morrison J QUANTO 1.1: A computer program for power and sample size calculations for genetic-epidemiology studies. Available at http://biostats.usc.edu/Quanto.html; Accessed on September 2014.
Campa D, Gioia A, Tomei A, Poli P, Barale R . Association of ABCB1/MDR1 and OPRM1 gene polymorphisms with morphine pain relief. Clin Pharmacol Ther 2008; 83: 559–566.
Mura E, Govoni S, Racchi M, Carossa V, Ranzani GN, Allegri M et al. Consequences of the 118A>G polymorphism in the OPRM1 gene: translation from bench to bedside? J Pain Res 2013; 6: 331–353.
Oertel BG, Schmidt R, Schneider A, Geisslinger G, Lotsch J . The mu-opioid receptor gene polymorphism 118A>G depletes alfentanil-induced analgesia and protects against respiratory depression in homozygous carriers. Pharmacogenet Genom 2006; 16: 625–636.
Romberg RR, Olofsen E, Bijl H, Taschner PE, Teppema LJ, Sarton EY et al. Polymorphism of mu-opioid receptor gene (OPRM1:c.118A>G) does not protect against opioid-induced respiratory depression despite reduced analgesic response. Anesthesiology 2005; 102: 522–530.
Hayashida M, Nagashima M, Satoh Y, Katoh R, Tagami M, Ide S et al. Analgesic requirements after major abdominal surgery are associated with OPRM1 gene polymorphism genotype and haplotype. Pharmacogenomics 2008; 9: 1605–1616.
Huehne K, Leis S, Muenster T, Wehrfritz A, Winter S, Maihofner C et al. High post surgical opioid requirements in Crohn's disease are not due to a general change in pain sensitivity. Eur J Pain 2009; 13: 1036–1042.
Kroslak T, Laforge KS, Gianotti RJ, Ho A, Nielsen DA, Kreek MJ . The single nucleotide polymorphism A118G alters functional properties of the human mu opioid receptor. J Neurochem 2007; 103: 77–87.
Connor M, Osborne PB, Christie MJ . Mu-opioid receptor desensitization: is morphine different? Br J Pharmacol 2004; 143: 685–696.
Dang VC, Christie MJ . Mechanisms of rapid opioid receptor desensitization, resensitization and tolerance in brain neurons. Br J Pharmacol 2012; 165: 1704–1716.
Kim KS, Lee KW, Im JY, Yoo JY, Kim SW, Lee JK et al. Adenylyl cyclase type 5 (AC5) is an essential mediator of morphine action. Proc Natl Acad Sci USA 2006; 103: 3908–3913.
Martini L, Whistler JL . The role of mu opioid receptor desensitization and endocytosis in morphine tolerance and dependence. Curr Opin Neurobiol 2007; 17: 556–564.
Johnson AD, Zhang Y, Papp AC, Pinsonneault JK, Lim JE, Saffen D et al. Polymorphisms affecting gene transcription and mRNA processing in pharmacogenetic candidate genes: detection through allelic expression imbalance in human target tissues. Pharmacogenet Genom 2008; 18: 781–791.
Oertel BG, Doehring A, Roskam B, Kettner M, Hackmann N, Ferreiros N et al. Genetic-epigenetic interaction modulates mu-opioid receptor regulation. Hum Mol Genet 2012; 21: 4751–4760.
Beyer A, Koch T, Schroder H, Schulz S, Hollt V . Effect of the A118G polymorphism on binding affinity, potency and agonist-mediated endocytosis, desensitization, and resensitization of the human mu-opioid receptor. J Neurochem 2004; 89: 553–560.
Oertel BG, Kettner M, Scholich K, Renne C, Roskam B, Geisslinger G et al. A common human micro-opioid receptor genetic variant diminishes the receptor signaling efficacy in brain regions processing the sensory information of pain. J Biol Chem 2009; 284: 6530–6535.
Zhang Y, Wang D, Johnson AD, Papp AC, Sadee W . Allelic expression imbalance of human mu opioid receptor (OPRM1) caused by variant A118G. J Biol Chem 2005; 280: 32618–32624.
Ray R, Ruparel K, Newberg A, Wileyto EP, Loughead JW, Divgi C et al. Human Mu Opioid Receptor (OPRM1 A118G) polymorphism is associated with brain mu-opioid receptor binding potential in smokers. Proc Natl Acad Sci USA 2011; 108: 9268–9273.
Bond C, LaForge KS, Tian M, Melia D, Zhang S, Borg L et al. Single-nucleotide polymorphism in the human mu opioid receptor gene alters beta-endorphin binding and activity: possible implications for opiate addiction. Proc Natl Acad Sci USA 1998; 95: 9608–9613.
Yildiz K, Tercan E, Dogru K, Ozkan U, Boyaci A . Comparison of patient-controlled analgesia with and without a background infusion after appendicectomy in children. Paediatr Anaesth 2003; 13: 427–431.
Gordon DB, Pellino TA . Incidence and characteristics of naloxone use in postoperative pain management: a critical examination of naloxone use as a potential quality measure. Pain Manag Nurs 2005; 6: 30–36.
Sinatra RS, Jahr JS, Reynolds LW, Viscusi ER, Groudine SB, Payen-Champenois C . Efficacy and safety of single and repeated administration of 1 gram intravenous acetaminophen injection (paracetamol) for pain management after major orthopedic surgery. Anesthesiology 2005; 102: 822–831.
Hiller A, Helenius I, Nurmi E, Neuvonen PJ, Kaukonen M, Hartikainen T et al. Acetaminophen improves analgesia but does not reduce opioid requirement after major spine surgery in children and adolescents. Spine 2012; 37: E1225–E1231.
Angst MS, Koppert W, Pahl I, Clark DJ, Schmelz M . Short-term infusion of the mu-opioid agonist remifentanil in humans causes hyperalgesia during withdrawal. Pain 2003; 106: 49–57.
dbSNP: the NCBI database of genetic variation. http://www.ncbi.nlm.nih.gov/projects/SNP/snp_ref.cgi?rs=1799971database on the Internet. 2001 [cited December 5th 2013]. Available from http://www.ncbi.nlm.nih.gov/projects/SNP/snp_ref.cgi?rs=1799971.
Lotsch J, Zimmermann M, Darimont J, Marx C, Dudziak R, Skarke C et al. Does the A118G polymorphism at the mu-opioid receptor gene protect against morphine-6-glucuronide toxicity? Anesthesiology 2002; 97: 814–819.
Landau R, Kern C, Columb MO, Smiley RM, Blouin JL . Genetic variability of the mu-opioid receptor influences intrathecal fentanyl analgesia requirements in laboring women. Pain 2008; 139: 5–14.
Song Z, Du B, Wang K, Shi X . Effects of OPRM1 A118G polymorphism on epidural analgesia with fentanyl during labor: a meta-analysis. Genetic Testing and Molecular Biomarkers 2013; 17: 743–749.
Sprouse-Blum AS, Smith G, Sugai D, Parsa FD . Understanding endorphins and their importance in pain management. Hawaii Med J 2010; 69: 70–71.
Acknowledgements
The project described was supported by the National Center for Research Resources and the National Center for Advancing Translational Sciences, National Institutes of Health, through Grant 8 UL1 TR000077 through the T1 Junior Faculty Award and Clinical Research Feasibility Funds (PI: Chidambaran). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH. It was also supported by the APSF / ASA Safety Scientist Career Development Award by the Anesthesia Patient Safety Foundation (PI: Chidambaran). We acknowledge the contributions of the Clinical Analytic support team at Cincinnati Children’s Hospital for their assistance with medical record data retrieval.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Chidambaran, V., Mavi, J., Esslinger, H. et al. Association of OPRM1 A118G variant with risk of morphine-induced respiratory depression following spine fusion in adolescents. Pharmacogenomics J 15, 255–262 (2015). https://doi.org/10.1038/tpj.2014.59
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/tpj.2014.59
This article is cited by
-
ABCC3 genetic variants are associated with postoperative morphine-induced respiratory depression and morphine pharmacokinetics in children
The Pharmacogenomics Journal (2017)
-
Morphine versus methylprednisolone or aminophylline for relieving dyspnea in patients with advanced cancer in China: a retrospective study
SpringerPlus (2016)
-
Sweet taste pleasantness is modulated by morphine and naltrexone
Psychopharmacology (2016)